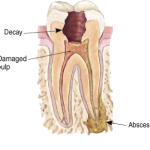
What is Endodontics?

Above definition credited to Wikipedia.
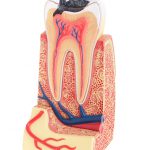
tooth anatomy (vital tooth, structure, bone, ligament)
What is the nerve?
Our teeth are hollow and at the center of your tooth is pulp, otherwise known as the “nerve.” The pulp is a collection of blood vessels that helps to grow the surrounding tooth. It is comprised of blood vessels, lymphatic systems, innervations, and connective tissue. Without these tissues, teeth
would never form. Once your tooth is formed, however, the pulp serves no developmental function. Yes, that is true. You don’t need the nerve to keep your tooth. Its real job is to tell us when we have damage to the tooth or the pulp itself. The health of a tooth does not depend on a living pulp. It depends, instead, on a healthy and living attachment (the periodontal ligament) to the surrounding bone and the host response (your systemic ability to heal).
Nonsurgical Root Canal Therapy
Infection of the pulp can be caused by trauma to the tooth, deep decay, cracks, or repeated dental procedures. Symptoms of the infection can be identified as visible injury or swelling of the tooth, sensitivity to temperature and biting, or spontaneous throbbing pain radiating to other parts of the jaw and facial structures like your ear or your temple. Root canal treatment successfully replaces the damaged delicate root canal system with an inert pulpal filling material. The damaged pulp is microscopically removed and the canals are prepared with measurable precision, disinfected with multiple irrigating solutions, and then freshly sealed with an inert three-dimensional filling material. Successful outcomes can be as high as 97% by an Endodontist with an accurate diagnosis.
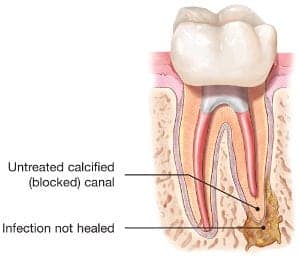
Nonsurgical Root Canal Retreatment / Revision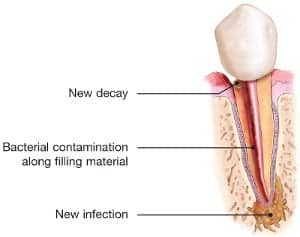
With the appropriate care, your teeth that have had endodontic treatment will last as long as other natural teeth. Yet, a tooth that has received treatment may fail to heal or continue to cause pain. This may occur from a new cavity approaching the root canal filling, a crack in the tooth, missed anatomy, anatomy that is physically impossible to mechanically cleanse, or a resistant infection. Sometimes, the pain may occur months or years after treatment. If so, endodontic retreatment may be needed. The existing root canal filling is microscopically removed and rechecked for any missing anatomy, re-disinfected with multiple irrigating solutions, possibley medicated, and then sealed with new filling material. This may be a frustrating event but it is a successful way to save your tooth from extraction. Successful outcomes for Retreatment are close to 90% by an Endodontist with an accurate diagnosis
Surgical Endodontic Therapy / Revision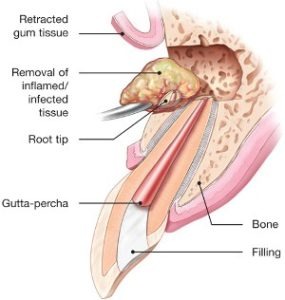
 Generally, a root canal or root canal retreatment is all that is needed to save teeth with an injured pulp from extraction. Occasionally, it will not be sufficient to heal the tooth. Surgery may then be recommended as the final attempt to save your tooth. Endodontic surgery is performed to locate fractures, hidden canals, or resorptive defects that do not appear on X-rays or under the microscope. Damaged root surfaces, damaged surrounding bone, and inflamed scar tissue may also be addressed during surgery. The most common surgery used to save damaged teeth is an APICOECTOMY or root-end resection. The root tip with attached infected tissue is physically resected, removed, and sealed microscopically. The procedure is similar to gum surgery or a surgical extraction. Other common Surgical Endodontic procedures include: Resorption Repair, Root Amputation, Hemisection, & Replantation. The doctors will review all possible complications and expectations with endodontic surgery as opposed to other options when conventional therapy is not successful. Endodontic apical microsurgery success can be as high as 90% by an Endodontist with an accurate diagnosis.
Generally, a root canal or root canal retreatment is all that is needed to save teeth with an injured pulp from extraction. Occasionally, it will not be sufficient to heal the tooth. Surgery may then be recommended as the final attempt to save your tooth. Endodontic surgery is performed to locate fractures, hidden canals, or resorptive defects that do not appear on X-rays or under the microscope. Damaged root surfaces, damaged surrounding bone, and inflamed scar tissue may also be addressed during surgery. The most common surgery used to save damaged teeth is an APICOECTOMY or root-end resection. The root tip with attached infected tissue is physically resected, removed, and sealed microscopically. The procedure is similar to gum surgery or a surgical extraction. Other common Surgical Endodontic procedures include: Resorption Repair, Root Amputation, Hemisection, & Replantation. The doctors will review all possible complications and expectations with endodontic surgery as opposed to other options when conventional therapy is not successful. Endodontic apical microsurgery success can be as high as 90% by an Endodontist with an accurate diagnosis.
Internal Bleaching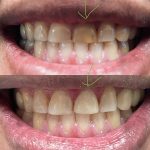
Internal bleaching is a technique that is used to whiten the appearance of teeth from the inside of a tooth. Internal bleaching is conducted under the direction of a dentist.The process for an internal bleaching involves the insertion of a bleaching agent inside the crown portion of the tooth. A root canal is necessary for internal bleaching. The bleaching gel is left in the tooth for several days, and may be replaced with more bleaching agents until the tooth achieves the level of whiteness desired. Once the series of treatments are complete, the hole is sealed, ensuring that foreign matter will not be able to invade the tooth. It is a conservative way of improving the esthetics of your front teeth without crowns or veneers.
Root canals seed infections in my body and contribute to systemic disease. Fact or Fiction?
FICTION. There are several websites and movies posing as legitimate documentaries questioning the validity of conventional root canal therapy. Beware that evidence can be found for anything you believe in and persuade you in either direction. Decades of research have debunked the focal infection theory findings. In other words, the theory blames root canal therapy as the cause in other chronic conditions and illnesses. The American Dental Association reviewed Dr. Weston Price’s (holistic dentistry) research techniques from the 1920s and noted that they lacked many aspects of modern scientific research, including absence of proper control groups and induction of excessive doses of bacteria. Root canal treatment is specifically designed to remove infection from the tooth and prevent it from spreading.
Why should I consider root canal therapy?
 Endodontic treatment (ROOT CANAL THERAPY) along with an appropriate restoration, is a cost-effective way to treat teeth with a damaged pulp. Retention of one’s natural dentition may also provide support to the nearby supporting hard and soft tissues. It is usually less expensive and complicated than extraction with placement of a bridge or an implant. Placement of a bridge or an implant will require significantly more time and complexity in treatment and may result in further procedures to adjacent teeth and supporting tissues. Those healthy teeth are helping patients chew efficiently, maintain the natural appearance of their smiles and enhance their enjoyment of life. Through endodontic treatment, endodontists and dentists worldwide enable patients to keep their natural teeth for a lifetime.
Endodontic treatment (ROOT CANAL THERAPY) along with an appropriate restoration, is a cost-effective way to treat teeth with a damaged pulp. Retention of one’s natural dentition may also provide support to the nearby supporting hard and soft tissues. It is usually less expensive and complicated than extraction with placement of a bridge or an implant. Placement of a bridge or an implant will require significantly more time and complexity in treatment and may result in further procedures to adjacent teeth and supporting tissues. Those healthy teeth are helping patients chew efficiently, maintain the natural appearance of their smiles and enhance their enjoyment of life. Through endodontic treatment, endodontists and dentists worldwide enable patients to keep their natural teeth for a lifetime.
Does root canal therapy work?
 Root canals can SAVE your teeth, your bite and your smile. Otherwise, the alternative is LOSS of your tooth and consideration for a missing tooth with dentures, implants, or bridges. Uncomplicated root canal therapy by an Endodontist is roughly 95% successful. That means, 1 out of every 20 root canal treatments will fail. A positive outcome depends on your ability to heal (host response), existing bone support, remaining tooth support and the gums around the tooth. Complications, such as root fractures, infection, bruising, perforations, obstructions, calcified canals, severe curves, instrument fracture, prior root canal treated teeth, prior doctor error, trauma, resorption, complex restorations, complex anatomy, deep decay, minimal remaining tooth, the inability to thoroughly clean the canals, failure to restore the tooth in time, and other things may hinder the success rate. We STRIVE to provide the best care to save your teeth, however, COMPLICATIONS in outcome may arise under the most ideal treatment settings. We strive for success yet, treated teeth may need a surgery, revision or still extraction. These are additional procedures that are not included in the cost of the prior treatment. Surgery and retreatment/revision do have a lower success rate than the initial root canal therapy but is still a excellent alternative to extraction and saving your tooth.
Root canals can SAVE your teeth, your bite and your smile. Otherwise, the alternative is LOSS of your tooth and consideration for a missing tooth with dentures, implants, or bridges. Uncomplicated root canal therapy by an Endodontist is roughly 95% successful. That means, 1 out of every 20 root canal treatments will fail. A positive outcome depends on your ability to heal (host response), existing bone support, remaining tooth support and the gums around the tooth. Complications, such as root fractures, infection, bruising, perforations, obstructions, calcified canals, severe curves, instrument fracture, prior root canal treated teeth, prior doctor error, trauma, resorption, complex restorations, complex anatomy, deep decay, minimal remaining tooth, the inability to thoroughly clean the canals, failure to restore the tooth in time, and other things may hinder the success rate. We STRIVE to provide the best care to save your teeth, however, COMPLICATIONS in outcome may arise under the most ideal treatment settings. We strive for success yet, treated teeth may need a surgery, revision or still extraction. These are additional procedures that are not included in the cost of the prior treatment. Surgery and retreatment/revision do have a lower success rate than the initial root canal therapy but is still a excellent alternative to extraction and saving your tooth.

After root canal therapy…
During root canal therapy, existing dental work may be destroyed. Fillings are routinely removed. The original dental work may need to be redone by your family dentist. Most teeth which have root canal therapy will require a new crown placed by your family dentist. Please contact your general dentist after care is completed for further recommendations. What to expect after care and after-pain management strategies are enclosed in your patient packet. Do not hesitate to contact us. Sometimes, a simple phone call will clarify any concerns.